Why HCM?
If you have read the “About” page of this blog, or if you know anything about me and my story, you know that I have faced several serious health challenges in my life, of which HCM is only one. In fact, HCM has not even been responsible for the most serious health crisis of my life to date. However, HCM holds a very significant place in my life, and the words that follow will explain to you the reasons for this significance. HCM’s impact on me and my family, generation after generation, is the force that moved me to create this website, form several HCM support groups both online and in my community, and to volunteer my time and expertise helping related non-profits. If you would like to know all the ins and outs of my story, then read on.
The first time HCM entered my life, though I didn’t know what it was called yet, I was six years old. I was playing in my bedroom in our house in New Orleans when my mother ran in. She told me to go get the next door neighbor, a doctor, because my father had collapsed and my mom didn’t know what to do. Dr. Bresler wasn’t home, so my mom called 911, and my dad was taken away in an ambulance. At the hospital they patched him up, and sent him back home a day or so later.
The next time the still nameless enemy entered my life, my family was caught totally unprepared. I was nine. My father, my three cousins and I were visiting my grandmother in Boston, just as we did every summer. I had just taken my turn playing Clue. My guess was that Col. Mustard did it with the Candlestick in the Study. Then I heard the telephone ring. We heard a shrieking noise coming from the other room. I thought that it was someone having a good laugh. Instead, it was my grandmother, hysterical because she had just been told that my father’s brother, her eldest son, had drowned in Los Angeles while swimming in the Pacific Ocean.
Years later when I reviewed his autopsy report while researching my own diagnosis, I would find out that the coroner measured his septum at 1.8 cm. and the slides taken from his heart showed extensive interstitial fibrosis, yet he was diagnosed with “hypertensive cardiomegaly” despite having no personal or family history of hypertension. He left 3 young kids fatherless. No one could ever figure out why my uncle, a strong swimmer, drowned while taking the same swim he took every day.
Meanwhile, my father’s syncope episodes continued throughout my childhood. When I was eleven, my father collapsed again at home, after bringing in the garbage cans from the street. Again, I was sent off to retrieve a different doctor/neighbor, and again, another ambulance hauled my father off to the hospital.

When I was in high school, I was called into the principal’s office one afternoon and told that my father had suffered a major stroke and had been brought to the hospital. I hurried to his bedside after school and was terrified to see him in that condition – unable to speak or move.
Eventually my dad regained most of his motor functions and was able to resume a fairly normal life – at least for a while. And I went on with my life. I went to college, law school, and moved out to Los Angeles to start my life as an adult.
No one ever suggested to my family that my father’s condition was hereditary. It was known that he had “IHSS” which is a now outdated term for HCM as he was formally diagnosed in the late 1960s. In fact, when I was a young child, my mother was told that IHSS usually only presented in males, so I was safe.
My mom always kept her Merck Manual within easy reach. So, years later, when a cardiologist friend casually mentioned to my mother that he thought that my uncle had died of the very same IHSS which afflicted my father, my mom pulled out her trusty Merck Manual. She learned that IHSS was now called HCM, and was passed along in an autosomal dominant fashion. My mom immediately called me and told me what she had learned from her consultation with Dr. Merck. She suggested that I look into getting checked out. I told her that I was too busy working at my studio legal affairs job which required me to work late every night, plus weekends, but that I would look into it whenever I had some free time.
A few months later, a friend happened to mention her cardiologist. Since she spoke so highly of this doctor, I thought that it might be the time to make that appointment. And, when I thought back over the last few years, I recalled that one doctor had mentioned hearing a murmur and I did notice little flutters in my chest from time to time, so I resolved that I would look into things further when time allowed.
My visit went fine, or so I thought, because that doctor told me that I didn’t have the same thing as my dad. However, he asked me to return to his office for an echo to make sure that everything was ok. Upon reviewing my medical records years later, I discovered that the EKG taken during that first appointment was read as abnormal, consistent with left ventricular hypertrophy.
The echo showed that I was not obstructed, and I didn’t have any mitral valve regurgitation, so I was put on an annual visit schedule and was told that we would just follow my condition every year to make sure that nothing had changed.
At that time, I was not placed on any medication nor were my activities restricted in any way. My doctor considered me “asymptomatic.” He did not think that there was any reason to go on medication without symptoms and he assured me that my situation wouldn’t prevent me from leading a normal life. He even cleared me to exercise with a trainer without restrictions since at the time, I was planning my wedding and wanted to be in great shape for the big walk down the aisle.
In the old days, the only way for patients to collect information about health conditions, besides whatever information they were directly given by their doctors, was to visit libraries and book stores and read whatever information they could find on the shelves. With the advent of the internet, information gatherers like me were given an amazing gift and tool for advancing their health care. And this was right up my alley! I had been well trained as both a researcher and a decision maker. In fact, the first job of my career after law school was as a law clerk to a respected Superior Court Judge.

After my diagnosis in 1999, I went searching for information on the internet and I came up with some invaluable resources. I began to read and read and read some more. I learned who the top HCM researchers were, and what they were saying. Being newly married, the big one on my mind at the time was could I have children? My husband and I had been planning a family, but now I wasn’t so sure. Could I safely carry and deliver a child? And what about the hereditary nature of the disease? Could I live with myself if I gave birth to a child with HCM? Ultimately, my research helped me find the information my husband and I needed to make this important decision, and satisfied with our decision, we proceeded with our new undertaking.
I was able to get pregnant quickly, and had a fairly routine pregnancy, though my shortness of breath and palpitations did increase. Throughout, I was followed by a perinatologist, cardiologist and OB. Despite the precautions, following an epidural, I passed out twice and my BP fell to 50/30, but luckily with fluids and bed rest, I was back to normal, at least for a little while!
I went home with my new son, and for the next eight or so weeks, we led a blissful existence. No sleep, fountains of urine directed at my face, milky barf on every piece of clothing.
The only problem was that I just couldn’t shake a sinus infection. My right ear was blocked up and I kept having headaches. While on a short trip to New Orleans to introduce the baby to my father, the headaches took on a new urgency.
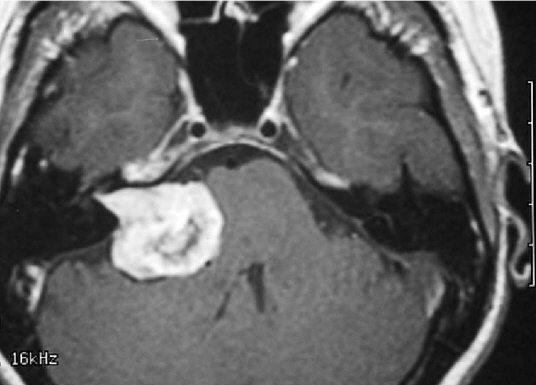
Upon my return to Los Angeles, I immediately wound up in the ER with hydrocephalus caused by a 3+ cm. acoustic neuroma compressing my brain stem by 50%. Two surgeries: one to implant a VP shunt and another to resect the tumor, left me in tip top shape – well…..except for the inconvenience of becoming totally deaf in one ear, and a few other minor annoyances such as inability to see straight, walk without listing to the right, close my eye, swallow — but I won’t bore you with that whole story.
My cardiologist had toyed with the idea of putting me on a small dose of beta blockers during my pregnancy, but I had resisted for fear of harming the baby. Now he thought it might be a good time to start the meds since it was evident that my days of breastfeeding were at an abrupt close.
My months of rehabilitation following the brain surgery were fairly routine from a cardiac perspective, until about 10 months later when I almost fainted when walking off the elevator in my condo building. I called my cardiologist who referred me to an E.P. in his practice. The E.P. recommended that I wear an event monitor for a week which didn’t turn up anything too interesting. Then, he recommended I undergo an E.P. study to evaluate my need for an ICD. Having become a regular on the HCMA website, I questioned him. Isn’t it true that E.P. Studies are of questionable benefit in HCM patients I asked? Well, he said, “it is still the right thing to do in your case. If you don’t agree, you can get a second opinion.”
So, that is what I did. I got THREE. Meanwhile, I continued to wear the event monitor. Over a 4 week period I was found to have multiple episodes of v-tach lasting 7 – 10 beats each. Ultimately, none of the other 3 doctors recommended that I proceed with the E.P. Study, but they did all agree on one thing –based on my risk factors, an ICD was a good idea.

One of my biggest concerns relating to the implantation of the ICD was that I would be giving up the ability to have an MRI. Having recently ridden on the brain tumor merry-go-round, I wasn’t too excited by the prospect of losing my ability to undergo MRI to follow my tumor. So, I also had to have my neurosurgeon weigh in on the matter.
He advised that while not optimal, a CT scan would be an adequate substitute.
I was on my way to becoming bionic!
Several friends had long recommended another well-known local E.P. to me, so I made an appointment to see him. I walked into his office with my now voluminous file and put it on his desk. Within ten minutes of meeting him after hearing him describe how he would implant the device, I told him to go ahead and schedule the procedure. I knew that he was the right doctor for me.
During that first consult, my new E.P. recommended that I adopt one of the specialists I had recently seen as my regular cardiologist. So, it was at that point I became a regular patient of a new cardiologist, an expert echocardiographer at a nearby teaching hospital.
I got my Medtronic dual chamber device in the beginning of 2003. My device was also programmed to provide backup pacing while my beta blocker dosage was increased. You see, the experts had discovered that in addition to the arrhythmias I was experiencing, I also had a large outflow tract gradient which occurred after exercise.
My symptoms began to sharply increase in the years after my son was born. My shortness of breath gradually began to worsen to the point where I was unable to walk up the slightest grade without feeling short of breath. Chest pain became my constant companion. I avoided walking up stairs whenever possible. For years, I tried increasing doses of beta blockers until I ultimately maxed out on the dosage.
With medical options diminishing, it was suggested that I might want to try having a septal alcohol ablation. After much consideration and discussion with my doctors, it was instead decided that I would try adding disopyramide (brand name Norpace) to my drug regimen.

Lucky for me, the timing of the decision to start taking the Norpace coincided with yet another surgical experience– the replacement of my ICD after two years due to a defective generator! I was able to combine both of these experiences with just one weekend away at the hospital. I thought of it as a weekend at the spa – away from the family with time to watch movies, read books, eat hospital food, take Tylenol and drink plenty to take care of that dry mouth.
The Norpace helped for a while, but it seemed that every dosage increase would improve the symptoms for a while, but the effect would ultimately peter out. Meanwhile, those particularly pleasant side effects became more pronounced.
Having spent many hours comparing notes with other HCM patients, I had a gut feeling that my situation was not going to improve without a major intervention. With this in mind, I decided to travel across the country to attend the annual HCMA Meeting.
There, I had the opportunity to meet the top experts in the field in person, including the HCM doctors from the Cleveland and Mayo Clinics, both top centers for clinical treatment as well as for septal reduction. I spent the weekend hearing all of the latest research and recommendations and went home with my head swimming with information. I also got to spend some time discussing my case with the Director of the HCM Clinic at Mayo, Dr. Steve Ommen.
By attending the meeting, and by doing LOTS of research, I learned that alcohol ablation is not the preferred type of septal reduction for patients who are otherwise young and healthy enough to undergo open heart surgery. I learned that if there are any mitral valve abnormalities, or if the obstruction is not located where the septal perforators route the alcohol, that ablation will not work. I learned that myectomy has a 30+ year proven track record, while alcohol ablation is relatively new and has been performed with mixed results. Plus, ablation leaves scar tissue in the heart which might cause arrhythmia. But what was most shocking to me was that alcohol ablations carry a mortality risk of about 5%, while for septal myectomy at an experienced center, the risk of mortality is less than 1%.
I spoke to numerous other patients who had undergone septal myectomies. Most had been able to resume their active lifestyles, though they had been debilitated by their pre-surgery conditions.
Meanwhile, the published literature was making my decision easier. In 2003, Dr. Martin Maron of Tufts/New England Medical Center published an article stating that patients who had outflow tract gradients of more than 30 millimeters of mercury had a much greater probability of death – Class III or IV heart failure, or stroke – than a patient who was not obstructed.
Two years later Dr. Ommen and his Mayo Clinic colleagues published another article finding that patients who had undergone septal myectomy had a life span equivalent with that of the average American. Those two studies taken together really had a strong impact on me.
So, now I had my job cut out for me. I had to sell my plan to my local doctors. I was up to the task, however. I sent them e-mails of abstracts and showed up at appointments with reading material for them to peruse in their spare time. I would pepper appointments with tidbits of wisdom that I had picked up from message boards and various articles. But most of all, I convinced them that I was unhappy with my quality of life. With good reason, they were cautious of sending a seemingly healthy person off to Minnesota to be cracked open like a nut. But the main issue and reason for my decision to go forward with the surgery was that I was not willing to spend my son’s childhood as an effective invalid. If there was a chance for me to grab the brass ring, I wanted to reach for it.

So, on August 11, 2006, I underwent an extended septal myectomy at the Mayo Clinic in Rochester, MN. The surgery went as planned, and Dr. Joseph Dearani was able to reduce my outflow tract gradient from over 100 mm of mercury to 0 mm of mercury.
Because I have concentric hypertrophy and my biggest area of obstruction was in the mid-cavity, Dr. Dearani warned me that he might have to make a second incision through the apex of the heart in order to remove enough muscle to get rid of the bulge protruding into my left ventricle. Luckily, he was able to remove the entire area through the aortic valve and a second incision was not required.
My recovery from surgery was pretty average And, let me tell you, compared to recovery from brain surgery, recovery from open heart surgery is NOTHING
Within a month after surgery, I was able to walk the hills in my neighborhood with considerably less discomfort than before. Suddenly, I could eat my evening meal without feeling like an elephant was sitting on my chest for the rest of the night. It took a little while to get my strength back, and I slowly started increasing my exercise, but within a couple of months, I was back at work, was able to increase my efforts at the gym, and most importantly, I could go on outings with my family and not have total anxiety at the first sighting of a staircase or hill.
It has now been close to ten years since my surgery. If you compare echocardiograms of my heart from before the surgery and now, they look like they were taken of a different person. However, I am still aware that my surgery was not a cure. I know that I will take medication and need to have maintenance for the rest of my life. But I am a whole lot better than I was before I went through the surgery. And, I am lucky to have the support of my local doctors on a daily basis while the experts at Mayo are there for consultation if and when I need them.
Because of my own experiences related to HCM, and those of my family, I consider it to be my personal mission to help to get the word out about HCM, and to help other families and patients who are struggling with this disease and its consequences.
The health care system in the United States today is not set up to provide patients with the support that is needed; especially for those of us who have to learn how to manage a chronic condition. If patients want to get the best treatment, it is incumbent upon them to take an active role in their own care. It is my sincere hope that this website, and other resources like it, will help HCM patients and their families find their own way through this wilderness.
© 2016 Cynthia Burstein Waldman

